Does Glaucoma Cause Blindness?
When you receive your glaucoma diagnosis, it’s natural to wonder, “Will I go blind?” The truth is that many factors impact the answer to whether glaucoma will cause blindness for you or not. If left untreated, glaucoma will most likely lead to blindness, though it progresses slowly over the years.
What affects whether I go blind or not?
When treated, there is still uncertainty on whether glaucoma will cause blindness for you or not.
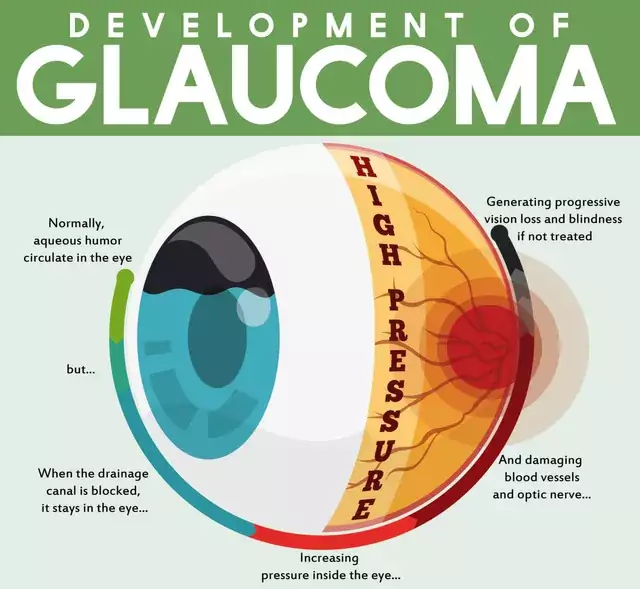
This is due to several variables, which include:
- what kind of glaucoma you have;
- what other risk factors and conditions you have that may complicate your glaucoma diagnosis;
- how much damage was already done by the time treatment began; and
- how compliant, proactive, and engaged you are in your treatment, supportive eye care, and utilization of low-vision aids, financial assistance, and other available resources.
In order to prevent going blind from glaucoma, it’s important to be proactive about your diagnosis and treatment.
What kind of glaucoma do you have?
The most common form of glaucoma among adults in the U.S. is open-angle glaucoma (OAG). OAG is a slow-progressing neurodegenerative disease that damages your optic nerve and destroys the retinal ganglion cells that connect your eye to your brain and control your vision. Your peripheral (side) vision is generally affected first. It can take years before your central vision is affected.
Another type, called angle-closure glaucoma (ACG), can cause a sudden attack that may result in total blindness within a matter of days if not treated as a medical emergency. A third type, normal-tension glaucoma (NTG), doesn’t cause sudden acute attacks, but it can damage your retinal cells faster than open-angle glaucoma and affect your central vision sooner.
What risk factors and other conditions apply to you?
Certain risk factors and related medical conditions can influence whether or not you develop glaucoma, when you develop it, and how fast it progresses.

Research shows that Black people should start getting tested for glaucoma at age 40—at least 20 years sooner than other racial groups.
(This image is by @mego-studio on Freepik.)
These risk factors and conditions include the following:
- Black, Hispanic, or Asian racial groups
- age 60 or older (lowers to age 40 or older for Black racial group)
- family history of glaucoma
- diabetes, high blood pressure, and/or other medical conditions
- nearsightedness
- history of eye trauma or steroid use
How much damage occurred before treatment?
Glaucoma typically affects the peripheral (side) vision first, specifically in OAG. These changes may go unnoticed for quite some time because the unaffected eye can compensate for the affected one.
There are pros and cons to your body’s ability to adapt to this situation. On the one hand, it’s fortunate, because it means that you may not suffer any vision loss in the early and moderate stages of the disease. It’s possible for your central vision to remain at 20/20.
The drawback, however, is that since you’re not experiencing vision loss in the early or moderate stages, you may not go to the eye doctor until significant irreparable damage has already been done. The earlier that glaucoma is diagnosed and treated, the greater your chances are of retaining a good portion, or even all, of your vision.
How engaged are you in your treatment process?
Going for regular eye exams is your first and best defense against going blind from glaucoma, as it increases your chances of getting an early diagnosis.

Eye drop medications are one of the common types of glaucoma treatment.
(This image is from Freepik.)
Once you’ve received a diagnosis, however, you must stay dedicated to the treatment process, which includes the following steps:
- Comply with every aspect of your prescribed treatment and supportive eye care.
- Keep your follow-up exam appointments.
- Quickly let your eye doctor know of any vision changes you experience.
- Take advantage of visual rehabilitation, low-vision aids, financial assistance programs, and other available resources that will help you carry out and sustain your necessary treatment and care.
You may not have control over all of the factors that impact whether your glaucoma will cause blindness. You do, however, have the power to control some of them. Be sure to speak to your ophthalmologist about how you can best influence your outcome.

