Patient Readiness, Not Just Reach: How Responsum Delivers Screener‑Ready Referrals
When enrollment stalls, it’s rarely because you don’t have enough people at the top of the funnel, it’s because the people reaching your sites aren’t ready to say yes to the next step. This post tells the story of how a study team moved from a spreadsheet full of names to steady, screener‑ready referrals by changing the conversation patients had before the coordinator called.
Reach ≠ Readiness (and why that matters)
In clinical research outreach, “more” isn’t always “better.” Large top‑of‑funnel campaigns often deliver unqualified or uncontactable names that bury coordinators in follow‑ups, and stall randomization. The bottleneck isn’t pageviews; it’s patient readiness: clear understanding, informed interest, and real‑world ability to take next steps.
Responsum’s thesis: when people learn in a trusted community first, and understand eligibility, logistics, and protections, they move from curiosity to confident action. That’s the difference between a list of leads and a slate of screener‑ready referrals.
What “screener‑ready” means at Responsum
When we say screener‑ready, we mean patients who:
- Understand the opportunity (purpose, procedures, time commitments, risks/benefits in plain language).
- Meet preliminary criteria based on community‑appropriate pre‑screens.
- Are contactable (validated contact details + preferred contact window).
- Have addressed obvious barriers (transport, caregiver needs, location, digital access, language).
- Consent‑literate and prepared to ask informed questions during the site’s call.
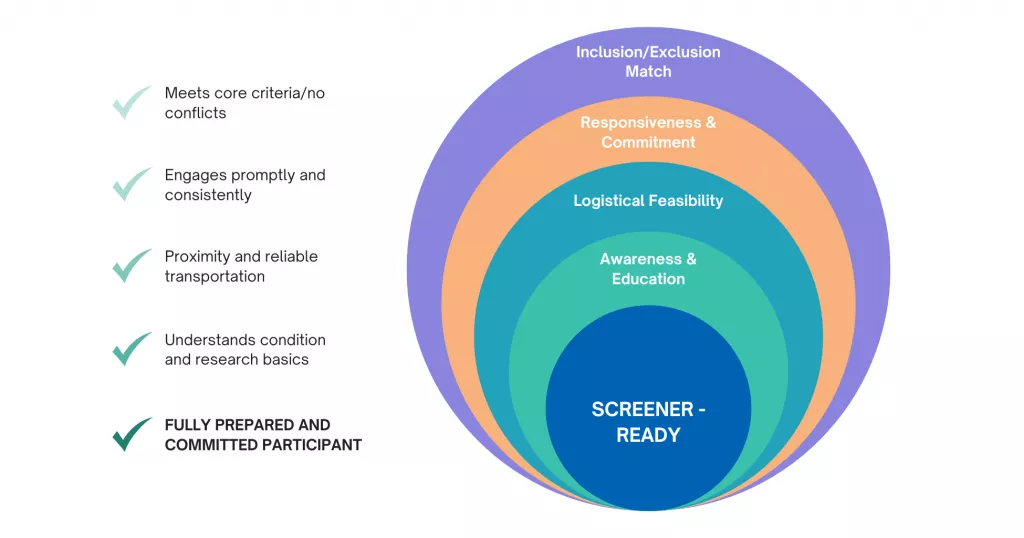
We engineer for these five outcomes inside our communities and content, before your site makes the first dial.
Our pre‑qualification pipeline (step‑by‑step)
Step 1: Awareness inside trusted communities.
We introduce opportunities with condition‑specific education (e.g., CKD, glaucoma, respiratory, CNS). Posts and resources are written in accessible, research‑grounded language and tuned for the questions patients actually ask.
Step 2: Plain‑language landing pages.
Pages clarify eligibility ranges, visit cadence, potential placebo, and participation expectations, reducing surprises that drive screen fails.
Step 3: Community‑fit pre‑screeners.
Short, inclusive pre‑screeners gather essentials (age range, diagnosis, meds, geography, key criteria red flags). We use branching logic to keep the experience fast and respectful.
Step 4: Readiness checks.
We surface practical barriers early: distance to site, transportation access, availability for visits, caregiver support, and device/internet needs for ePRO/televisits.
Step 5: Expectation setting & consent literacy.
Before handoff, we reinforce rights and protections (voluntary withdrawal, privacy, costs/compensation if applicable) and supply a short question guide patients can bring to the site call.
Step 6: Handoff with context.
Only patients who clear pre‑qualification, confirm interest, and opt‑in to share details are forwarded as screener‑ready referrals.
What your sites receive at handoff
Each referral includes a concise Referral Snapshot for coordinators:
- Contact info + preferred contact times
- Key pre‑screener fields (age range, diagnosis/status, relevant meds/criteria)
- Site proximity/transport notes
- Caregiver involvement (if applicable)
- Language/accessibility considerations
- Patient’s top 1–2 questions captured during pre‑screen
Coordinators can triage quickly, focus calls, and document outcomes in your CTMS with fewer back‑and‑forths.
The data you can see (portal transparency)
Partners get access to a shared view of the funnel, including:
- Traffic → pre‑screener starts/completions
- Pre‑qualified rate & reasons for disqualification
- Referral volume by site & week
- Contactability/connection rates
- Site feedback loop (screen outcomes where shared)
This transparency helps you tune criteria, identify friction, and allocate budget to the geos/sites converting best.
The update our sponsor actually cared about
Two weeks after launch, we walked the sponsor through a different kind of report, not a CTR victory lap, but the story of how readiness changed the downstream work for coordinators. Instead of impressions and clicks, we showed:
- % Pre‑Qualified: the share of starts who matched preliminary criteria after community education, not cold ads.
- % Contactable & Contact Rate: verified numbers and email health, plus first‑call connection outcomes captured by sites.
- Show Rate to Phone/On‑site Screen: scheduled screens that actually occurred once expectations were set.
- Screen Pass Rate: how many moved past formal screening as consent literacy improved.
- Time‑to‑First Referral: days from go‑live to the first qualified, coordinator‑ready handoff per site.
Those numbers told a simple story: when patients understand the why, what, and how, before they talk to a site, screening becomes a conversation, not a surprise. Coordinators get time back, sponsors get predictability, and enrollment stops lurching.
Equity built in: Transportation, tech, and trust
Readiness isn’t just eligibility; it’s logistics. We proactively:
- Flag transportation barriers and share available options (e.g., public transit routes, ride resources where appropriate)
- Provide caregiver‑friendly resources and visit planning tips
- Localize content and support inclusive language to broaden reach without diluting criteria
The result: fewer avoidable screen fails due to fixable, non‑medical obstacles.
Privacy, consent, and compliance
Responsum takes privacy seriously. We:
- Collect only the data necessary to qualify and connect patients
- Gain explicit opt‑in consent prior to any handoff
- Store and transmit referral data securely with least‑privilege access
- Provide clear patient education about rights, withdrawal, and data handling
This builds patient trust and simplifies collaboration with your sites and vendors.
From ghosts to green lights: a three‑week arc when saving a study
Week 0—Intake. Gather site pain points, audit prior ad and landing copy, and map the actual barriers candidates raised: travel, time commitment, placebo anxiety, and appointment logistics.
Week 1—Launch the pivot. Inside the relevant condition communities, lead with education instead of urgency: what the study asks of participants, how placebo works, why screens matter, and what to ask in the coordinator call. A 3‑minute pre‑screener uses branching logic to check preliminary criteria and surface transport constraints.
Week 2—Readiness shows up. Referral snapshots arriving at the sites include preferred contact windows, travel notes, and the patient’s top question. Coordinators report fewer “who are you again?” calls and more focused, 10–12 minute conversations.
Week 3—Momentum. Calendars begin filling with kept screens, not just scheduled ones. First randomizations occur before month‑end. Budgets shift into the geographies converting best, and teams stop debating CTR in favor of readiness metrics.
We didn’t create demand out of thin air; we created understanding inside a trusted space, and sent only the people who raised their hands after they understood.
Getting started: Timeline & deliverables
Week 0–1: Setup
Discovery call, criteria review, site geos, content map, and KPI alignment. Build landing pages and pre‑screener.
Week 2: Launch
Go live across the relevant community and social channels; QA tracking; begin referrals.
Week 3+: Optimize
Weekly readouts (volume, quality, site feedback) with rapid content/criteria tuning.
You get:
- Content + pre‑screener assets
- Real‑time funnel view
- Qualified referrals with coordinator‑ready snapshots
- Weekly insights and recommendations
If you’re planning Q4 or laying groundwork for 2026 studies, let’s map a readiness‑first plan for your therapeutic areas. Book a 25‑minute discovery session and we’ll outline a tailored funnel, pre‑screener, and launch timeline.