National Kidney Month: Why Prevention is Critical, and How to Prepare for Emergencies
March is National Kidney Month! Most people now know about the importance of heart health, but fewer people think about the critical role that our kidneys play in our overall health and everyday lives. It’s vital that we think about it, though, because if our kidneys fail, then we need either dialysis or a kidney transplant to stay alive.
The theme of National Kidney Month 2023 is “Kidney Health for All: Preparing for the Unexpected, Supporting the Vulnerable.” In addition to the ongoing effort to encourage kidney screening and early detection of kidney disease, the 2023 campaign focuses attention on the impact that both natural and man-made disasters can have on people’s ability to access relevant:
- Diagnostic services,
- Treatments, and
- Care.
In order to appreciate the urgency of these situations, it helps to understand the numerous ways that our kidneys keep us alive and healthy.
How do our kidneys help us?
Our kidneys perform many jobs, among them:
- Filtering wastes from our blood. Wastes that are allowed to build up make our bodies toxic.
- Regulating our body fluids and blood pressure. Excess fluid buildup causes swelling, and strains the heart and other organs.
- Activating vitamin D and balancing minerals in our blood. These promote strong bones and healthy organ function.
Kidney failure affects every other function that our bodies perform to sustain life.
What causes kidneys to fail?
Sports like boxing, or serious car or work accidents, can cause acute kidney injury (AKI), but the majority of people with reduced kidney function are those living with some form of chronic kidney disease (CKD), a progressive condition for which there is currently no cure.
Diabetes, hypertension (high blood pressure), and heart disease are the top three causes of CKD. CKD, in turn, can also cause those three conditions. In fact, heart disease is the primary cause of death for people on dialysis with end-stage kidney disease.
Other causes of CKD and kidney failure include:
- Autoimmune diseases such as lupus and IgA nephropathy
- Genetic diseases like polycystic kidney disease
- Traumatic injuries
- Smoking
- Excessive alcohol consumption
- A consistently unhealthy diet, full of trans fats, salt, sugar, and other toxins that often lead to obesity, diabetes, hypertension, and heart disease
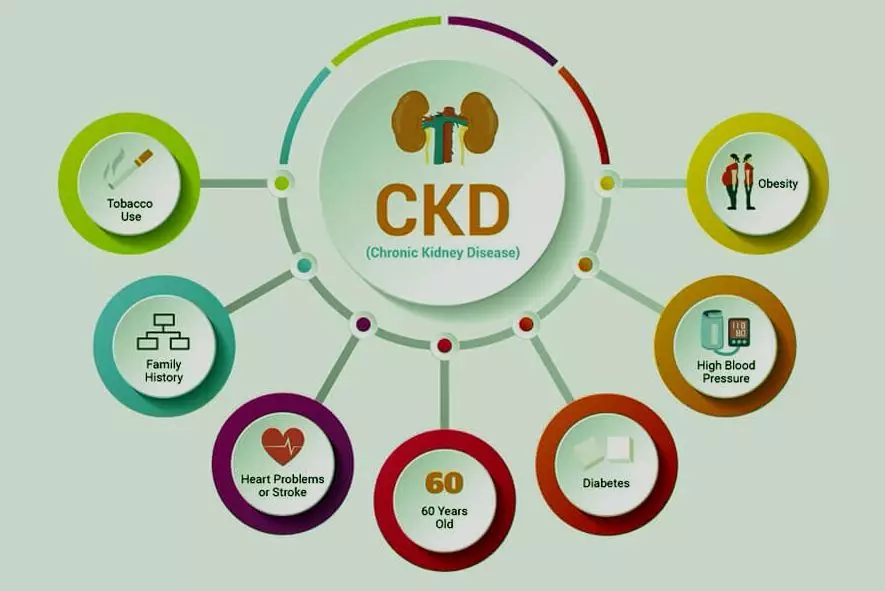
(Factors that can contribute to or influence the development of chronic kidney disease. Image from Atinu Critical Care Hospital)
All of these can place undue strain on your kidneys, overwhelming them and damaging them beyond repair. The best course of action is prevention, or at the very least early detection and intervention.
What can I do to protect my kidneys?
Generally speaking, kidney health is influenced by many factors, such as genetics, lifestyle habits, environment, and underlying medical conditions. Lifestyle factors are, by far, the easiest to control. Habits that support healthy kidneys include:
- Eating a diet of fresh fruits and vegetables, whole grains, and lean proteins,
- Getting regular physical exercise,
- Quitting smoking (or not starting), and
- Limiting alcohol consumption.
Getting screened regularly for indications of kidney disease, whether you’re at high risk or not, can also help prevent disease from developing, and/or halt its progression. Maintaining healthy kidneys is easier than fighting an active, progressive disease.

Maintaining a kidney disease care regimen can be even more challenging when a disaster or other emergency upsets and interferes with your access to medications, and to services like dialysis.
What can I do, as someone with CKD, to prepare for an emergency?
Disasters, both natural and human-made, can create complications for anyone, but especially for people who are medically vulnerable and dependent on life-preserving care. Planning ahead can help reduce fear and confusion, and smoothe the way for you to access alternative care and services. Here are some ways to plan for the unexpected.
Basics
- Keep an up-to-date list of your medications with you at all times, along with your insurance information.
- Stock up on your medications and diet needs at home—at least a two-week supply—and replace expired medications as needed.
- Have one or two portable phone batteries on hand, to keep your phone charged if your location loses power.
- Obtain and wear a medical bracelet with critical information about your condition.
- Keep a first aid kit and an emergency kit (your local police or fire department can make recommendations) on hand at home and at work.
Dialysis
Hemodialysis
Your regular dialysis center has an emergency plan. Learn what that is. In the case of a disaster, call your center to see if it’s open before venturing out. If you can’t reach your center, your local National Kidney Foundation (NKF) chapter may be able to tell you if your unit is open and operating.
Make a list of back-up dialysis providers and hospitals in your area, along with a back-up transportation plan, in case your usual center isn’t available. You can call the police or emergency services if you need immediate assistance.
The NKF suggests familiarizing yourself with ‘emergency diet’ protocols, in case you have to go without dialysis for a few days.
Peritoneal Dialysis
In addition to keeping a two-week supply of peritoneal dialysis equipment on hand, you may also want to:
-
- Keep the battery of your ultraviolet device charged (if you use one).
- Learn how to do CAPD exchanges, if you usually use a recycler.
- Learn how to stop dialysis in an emergency.
- Include a five-day supply of peritonitis antibiotics in your emergency pack.
- Register your name and address with your local water and power companies, so they prioritize your service restoration in case of an outage.
Transplantation
If you’re an organ transplant recipient, you can take the same precautions as dialysis patients, but there are several additional recommendations, as well:
- Keep your two-week supply of medications in their original bottles, if possible.
- Along with your medication list, pack the contact information for your doctor, pharmacist, transplant coordinator and insurance in a waterproof bag.
- In case you have to shelter with others, limit your exposure to infections by packing:
- Hand sanitizer,
- Gloves, and
- Masks.
It’s also a good idea to let any shelter staff know that you are a transplant recipient and need to take your medications on time. If you are caught in an emergency situation while away from home, you can contact the United Network for Organ Sharing (UNOS) 888.894.6361 for a list of transplant centers around the U.S.
Diabetes
If you have diabetes, make sure that you have the following packed and ready to go:
- Extra syringes and insulin
- A supply of glucose sources like honey, sugar, hard candy, juice, or glucose tablets
- Your blood sugar monitor, with extra batteries
- A copy of the diabetes emergency meal plan, and food supplies for several days
Anyone planning for an emergency could also benefit from packing:
- Bottled water
- Travel-sized toiletries
- Disposable eating utensils
- Dry clothes
- Flashlights and batteries
- A thermometer
- Canned and packaged food items that don’t require refrigeration
Click the link to download a PDF of the NKF Emergency Planning Guide, or contact FEMA for more general emergency-preparedness planning information.

