Treating Kidney Failure: Dialysis v. Transplant
Your kidneys filter excess fluid and waste products from your blood in order to avoid toxic buildup in your body and undue pressure on your heart and other organs. When kidneys fail, due to either severe injury or advanced disease, something else must take up the kidneys’ function in order to prolong life. Dialysis and kidney transplantation are the most common treatments for kidney failure, also called renal failure, but how do you decide which is best for you? Following is an overview of dialysis and transplantation, so you can have informed discussions with your healthcare provider about renal replacement before such treatment becomes necessary.
Types of dialysis
If your kidneys are no longer functioning, experts recommend that you start dialysis when you’re still feeling fairly healthy and your symptoms are still mild. Symptoms of kidney failure can include:
- Feelings of weakness and fatigue
- Difficulty concentrating
- Loss of appetite
- Nausea and vomiting
- Swelling in the face and limbs
There are two basic types of dialysis: hemodialysis and peritoneal dialysis. Your nephrologist (kidney doctor) can help you decide if and when to begin dialysis, as well as which type is best suited to you and your situation. Your blood and urine lab results, your overall health, and your personal preferences are all taken into consideration.
About hemodialysis
Hemodialysis can be performed at home or, as is common, at a dialysis center. Hemodialysis involves pumping your blood through a machine to remove waste products and excess fluids.
This is achieved through a fistula or graft, the surgical creation of a vascular access, which connects you to the dialysis machine.
In some cases, an alternative method may be used, in which a catheter (thin, flexible tube) is into a large vein in the neck or elsewhere in the body. Your blood is pumped into the machine, filtered, then pumped back into your body.
Sessions at a dialysis center generally take about three or four hours, and are performed an average of three times per week. In-center overnight sessions are also sometimes available. Hemodialysis sessions performed at home usually take between three and 10 hours, and are done three to six times a week.
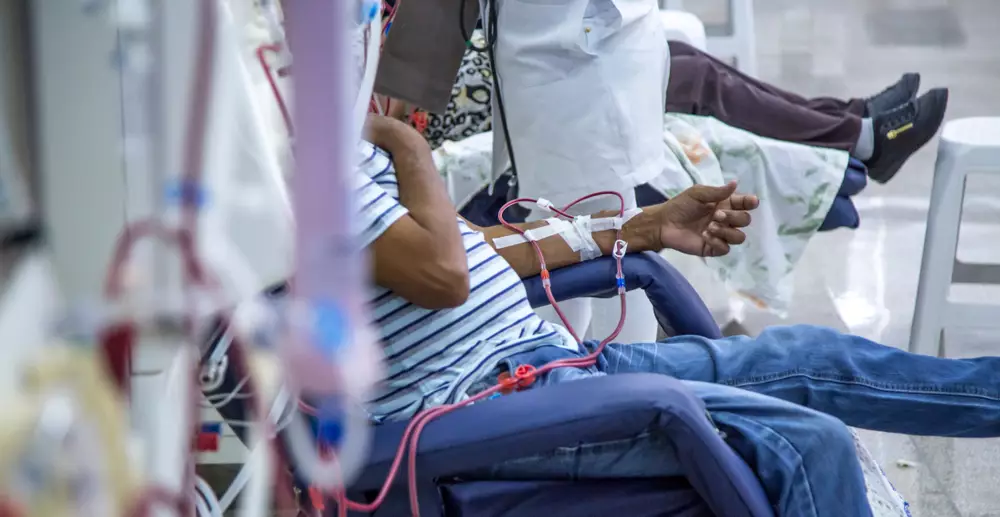
Pros and cons of hemodialysis
As with most choices, there are pros and cons to all options. Advantages of hemodialysis include typically brief treatments and little necessity for patient education regarding technical aspects of the process, as a dialysis technician or dialysis nurse will usually perform those duties unless you prefer in-center self-care and the center offers it.
Potential drawbacks of hemodialysis include:
- Physical symptoms during or after the dialysis session, such as:
- Lightheadedness
- Shortness of breath
- Abdominal cramps
- Nausea and vomiting
- Considerable time and energy investment in traveling to and from dialysis centers (if in-center
- Disruption of work and other activities if during the day, and family activities if at night
- Infections at the fistula site that can lead to sepsis
About peritoneal dialysis
Peritoneal dialysis, which is typically performed at home, involves filling your abdominal cavity with a fluid called the ‘dialysate’ (dye-AL-uh-sayt) through a catheter that is surgically inserted near your navel.
The fluid is usually held inside the abdomen for several hours, allowing excess fluids and waste products to be filtered out of the bloodstream. The waste-filled dialysate is then drained out of the abdomen and discarded, and the abdomen is refilled with fresh dialysate solution.
Peritoneal dialysis treatments may be done:
- By hand during the day (4-5 times)
- By machine (called a ‘cycler’) through the night while you sleep
- As a combination of nighttime cycler sessions and 1-2 daytime exchanges
Stay on top of your CKD
Responsum for CKD empowers people with kidney disease through community, knowledge, and shared experiences.
Pros and cons of peritoneal dialysis
Major advantages of peritoneal dialysis over hemodialysis are having fewer disruptions to your work, family time, and social activities.
Some potential disadvantages include:
- The learning curve involved in setting up the equipment, and self-administering the dialysis, including connecting and disconnecting the small tubes (having a family member or friend who can do this for you is helpful)
- Increased risk of hernia from the fluid pressure inside your abdominal cavity
- Potential weight gain
- Increased risk of infection at the catheter site (though this is rare)
Hemodialysis v. peritoneal dialysis
To-date, neither type of dialysis appears to have a clear advantage over the other regarding life expectancy. Your choice is mostly dependent on your personal preferences, overall health status, and home situation. You are also not locked in to one form of dialysis forever. It’s possible to switch forms as your preferences and life circumstances change.
About kidney transplantation

Kidney transplantation is the preferred treatment for many people facing or experiencing kidney failure. Transplant organs can come from living or deceased donors. During a kidney transplant, the surgeon places the healthy kidney in your lower abdomen and connects it to your bladder and blood vessels.
The non-working kidney is not necessarily removed unless it poses a risk to your recovery and overall safety. The procedure takes about three to four hours. Following the surgery, you will immediately be started on anti-rejection medications, and will likely spend several days in the hospital for observation.
Living v. deceased donor kidneys
Living donor kidneys are preferable, because they tend to function better, have a greater chance of being accepted, and function for longer periods of time (15 to 20 years) than deceased donor kidneys (10-15 years), potentially affording the recipient a longer and better quality life.
Having a willing living donor also means that you don’t have to potentially spend years on a transplant waitlist, during which time you would have to be on dialysis.
Pros and cons of kidney transplantation
The advantages of kidney transplantation are many, primarily:
- A healthy donor kidney can filter wastes from the blood more efficiently than dialysis can.
- The need for dialysis treatments is eliminated, saving time, energy, and life disruption.
- Recipients generally feel better after transplantation than after dialysis sessions.
Disadvantages of kidney transplantation include:
- A chronic organ shortage, leading to potentially long waits for up to 10 years, if you don’t have a willing living donor
- An extensive list of eligibility factors that must come together in order to qualify for transplantation
- The need to take daily medications for the remainder of your life, to ensure continued acceptance of the kidney
- The possibility that the kidney will be rejected immediately
- The usual risks of open surgery, including excessive blood loss, infection, and damage to nearby organs
Are there any other options?
Most people approaching end-stage kidney disease choose to undergo dialysis and/or kidney transplantation, but a third choice also exists: doing neither of those things. Some people, particularly if they are elderly or have other life-limiting medical conditions, choose something called conservative care, which focuses on preserving kidney function and quality of life until such time as hospice is called for.
It’s important to ask questions, and have informed discussions about your options and preferences with your family members and healthcare team, in order to make the best decisions for you.

