What Does an Effective Chronic Disease Care Plan Look Like?
If you or someone you care about has been diagnosed with CKD, it’s imperative that you work with your physician and care team to develop a comprehensive CKD care plan to address your unique medical and lifestyle needs. Having a clearly defined, realistic and executable care plan can help you reduce symptoms, address associated underlying conditions and maximize your health and quality of life. While a CKD diagnosis can often occur suddenly, and leave you scared and confused, it’s important to act immediately to prevent the onset of further damage. Here are some insights on developing a chronic kidney disease care plan that you can stick to and that works for you.
Mapping Out Your CKD Care Plan
You’ve just been diagnosed with CKD by your doctor; now what? Many people don’t even exhibit symptoms prior to their diagnosis, so it can be hard to know what to do next. The first step is identifying what stage of chronic kidney disease you’re in. CKD generally occurs in five stages, the extent of which are determined by something called your estimated glomerular filtration rate (eGFR). The lower your eGFR is, the worse your kidney disease is:
- Stage 1 CKD – eGFR of 90 or higher, which generally indicates some level of damage, although the kidney can still normally function.
- Stage 2 CKD – eGFR of 60-89, which usually indicates mild loss of kidney function.
- Stage 3 CKD (3a and 3b) – 3a is diagnosed with an eGFR of 45-49, indicating moderate decline and kidney function; 3b is diagnosed with an eGFR of 30-44, indicating severe decline.
- Stage 4 CKD – eGFR of 15-29, indicating escalation of decline to the point of failure.
- Stage 5 CKD – eGFR of less than 15, indicating failure or near failure of the kidney.
Knowing what stage of CKD you’re in will help you take the appropriate clinical and lifestyle steps to mitigate damage and maximize kidney function.

Image by Dmytro Zinkevych, Shutterstock.
Components of An Effective Care Plan
Figure Out What's Important
After determining what stage of CKD you’re in, you can determine your clinical and lifestyle priorities, including but not limited to:
- Your Career
- Your Ability to Travel
- Your Family Obligations
- The Kind of Activities You Enjoy
- Your Ability to Tolerate Treatment Side Effects
Ultimately, the most important element dictating your care plan will be your diagnosis. While someone in stage 1 CKD will not need dialysis, someone in stage 3b or above may require it. Talk to your doctor to balance the effectiveness of care versus your quality of life.
Start Eating a Kidney-Friendly Diet
No matter what stage of CKD you’re in, diet can help you to manage your symptoms. Generally speaking, a lower-sodium, plant-focused diet is best; however, for more serious cases, the DASH diet (Dietary Approaches to Stop Hypertension) can help stabilize blood pressure, lower the risk of cancer and other types of chronic illness that can worsen kidney function.
Stay Active…No Matter What
While your symptoms may stop you from achieving an intense level of exercise or physical activity, any level of movement can help you regulate weight and lower your BP. Work with your doctor to figure out how much exercise is advisable for your stage of CKD.
Keep Your Eyes Peeled for New Clinical Trials
More and more clinical trials are being conducted to advance quality of life and even reversal efforts of CKD. Keep working with your doctor to determine your eligibility and figure out the next steps to submit your participant application.
For CKD Healthcare Providers
Developing a CKD care plan depends on the immediate symptoms that patients are experiencing. There are specific protocols for CKD-related issues, such as:
- Excessive Fluid Volume
- Decreased Cardiac Output
- Nutritional Imbalance
- Fluid Deficiency
- Infection Control
Patients and doctors must keep working together to form the best chronic kidney disease plan available. While there are proven interventions and evidence-based best practices, each patient is unique and needs an individualized action plan.
Is Kidney Failure Reversible?
There are multiple types of kidney failure, including but not limited to:
- Acute Prerenal Kidney Failure – This type of kidney failure is caused by temporary insufficient blood flow. It is generally curable when your physician identifies the reason for the poor blood flow.
- Acute Intrinsic Kidney Failure – Acute intrinsic kidney failure results from the inability of kidneys to adequately filter waste from the blood, and in many cases, can be cured or reversed, as the origin is determined.
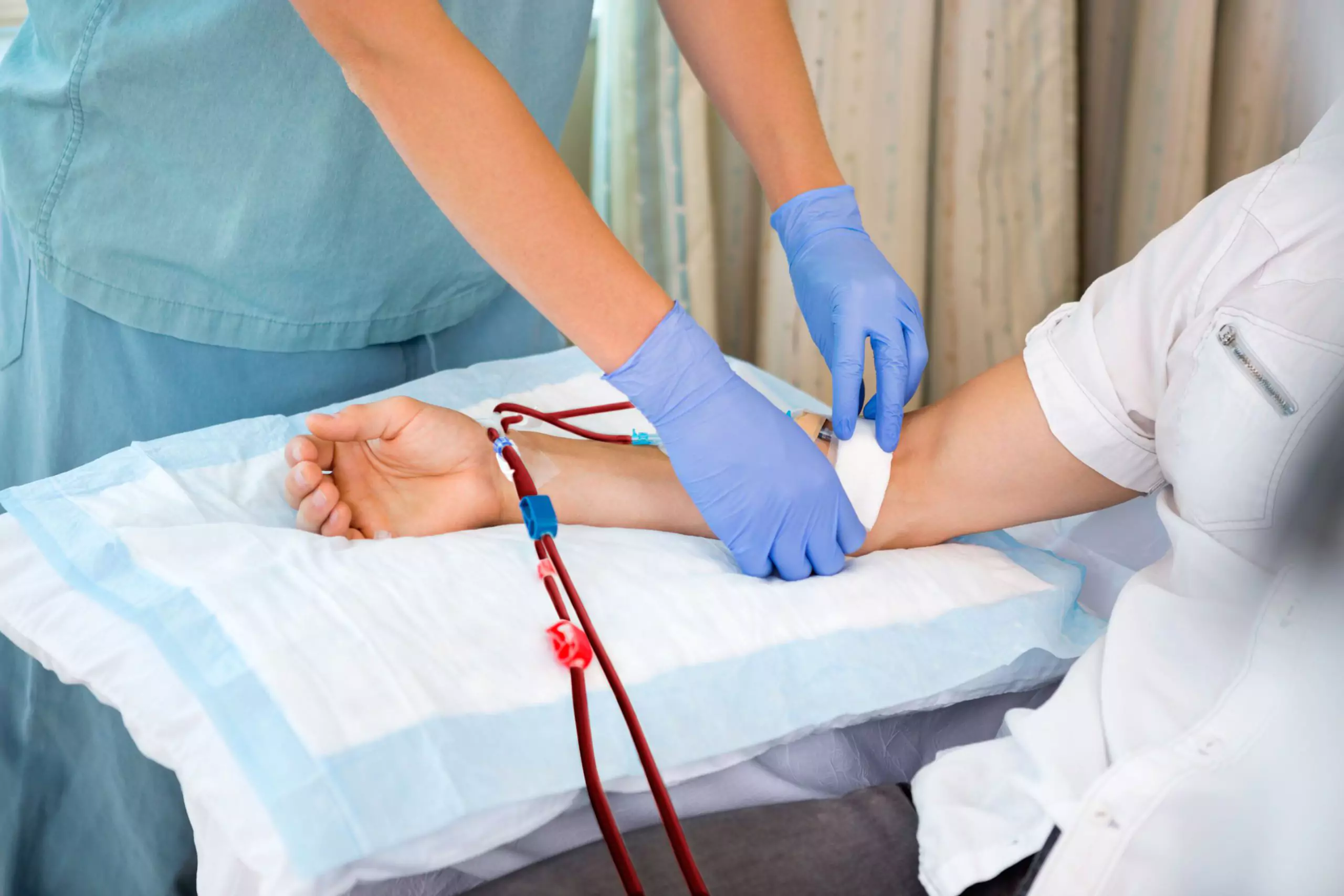
Image by Tyler Olson, Shutterstock.
Chronic kidney is more difficult to reverse and must be managed through proper symptom mitigation. Tests to determine kidney failure include, but are not limited to:
- Urinalysis
- Tissue Sample Extraction
- Urine Volume Measurements
- Blood Samples
- Imaging
There are five stages of kidney failure, the last of which signals increasingly urgent shut-down and failure of the organs and will likely require dialysis and transplant.
Working with Your Doctor to Manage Kidney Disease
While most types of kidney disease are not reversible, it’s still possible to maintain health and quality of life by working with your doctor and making lifestyle changes pertinent to your diagnosis. It’s important to realize that no two cases of kidney failure are the same, and you should continue to rely on your care team to provide the best course of care. Make and keep regular appointments, adopt a kidney-friendly diet, and make other everyday changes to lessen symptoms.


